In this article, we’ll delve into the controversial topic of gastrocnemius recession, an invasive surgery increasingly used to treat heel pain. We’ll explore the procedure, discuss its effectiveness, and weigh it against alternative treatments.
What Is Gastrocnemius Recession?
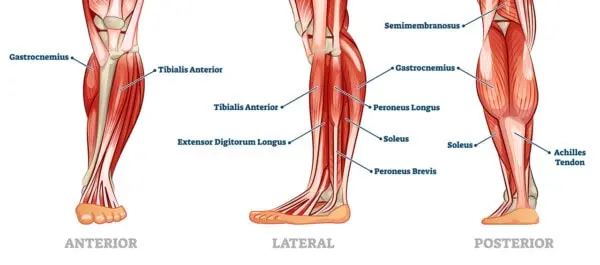
Gastrocnemius recession is a surgical procedure designed to alleviate heel pain. This pain often arises due to the tightening of the gastrocnemius, the calf muscle that connects the knee joint to the ankle. The tension can lead to discomfort in two areas: the back of the heel where the Achilles tendon attaches to the heel bone (calcaneus) or where the heel bone meets the ground (plantar fascia).
Many surgeons suggest that if conservative treatments like physical therapy or steroid injections fail to relieve this pain, gastrocnemius recession becomes necessary. This surgery aims to lengthen the calf muscle, thus reducing pressure on the affected area. But is this procedure really the best option, or are there less invasive alternatives?
PRP Research on Achilles Tendinopathy
The Achilles tendon links the calf to the heel bone, making it susceptible to damage when the calf is tight. This condition, known as tendinopathy, can cause significant discomfort. Platelet-rich plasma (PRP) therapy, a non-surgical approach, has gained popularity as a treatment.
A 2014 study by Filardo demonstrated favorable results with PRP injections, with follow-ups extending up to four years. A larger study in 2015 by Geulfi also reported excellent outcomes without resorting to surgery. The existing research hints at the effectiveness of PRP in treating Achilles tendinopathy.
PRP Injection for Heel Pain Due to Plantar Fasciitis
Plantar fasciitis is another common source of heel pain, caused by strain on the fascia at the bottom of the foot. Instead of invasive surgery, PRP injections have shown promise in alleviating this condition.
In a 2014 study, PRP outperformed steroid injections in treating plantar fasciitis. Several case series published in 2014 and 2015 also indicated the effectiveness of PRP in managing this condition. Furthermore, a 2014 study revealed that both dextrose prolotherapy and PRP were effective, offering non-invasive options for pain relief.
The Benefits of Gastrocnemius Recession
One of the primary benefits of Gastrocnemius Recession is pain relief. Patients often experience a significant reduction in foot pain, allowing them to return to their normal activities. Additionally, this surgery can improve flexibility and range of motion in the foot.
Potential Risks and Complications
As with any surgical procedure, there are risks associated with the Gastrocnemius Recession. These risks include infection, scarring, nerve damage, and the possibility of the procedure not achieving the desired outcome. It’s essential to discuss these potential complications with your surgeon before proceeding.
Recovery and Rehabilitation
Recovery from the Gastrocnemius Recession can vary from person to person. Physical therapy is often recommended to aid in the healing process and to regain strength and flexibility in the foot. It’s crucial to follow your surgeon’s post-operative instructions carefully.
Is Gastrocnemius Recession Right for You?
Determining if Gastrocnemius Recession is the right choice for you should be a collaborative decision between you and your healthcare provider. It’s essential to consider the severity of your condition, your lifestyle, and your willingness to undergo surgery.
Alternatives to Gastrocnemius Recession
Before opting for surgery, it’s worth exploring alternative treatments. These may include orthotics, physical therapy, and lifestyle modifications. Discuss these options with your healthcare provider to make an informed decision.
Cost of Gastrocnemius Recession
The cost of Gastrocnemius Recession can vary based on factors such as your location, the surgeon’s fees, and insurance coverage. It’s advisable to consult with your healthcare provider and insurance company to understand the potential costs involved.
The Research Base on Gastrocnemius Recession
As of now, there are only nine published studies on gastrocnemius recession to treat plantar fasciitis listed in the US Library of Medicine. Unfortunately, these studies fail to provide a strong basis for the procedure’s effectiveness. Most have only a three-month follow-up period, which isn’t sufficient to draw definitive conclusions about patient outcomes.
Crucially, there is a lack of randomized controlled trials, studies with biopsies, or research comparing the surgery to alternative treatments like PRP. This dearth of robust evidence challenges the assertion that gastrocnemius recession is a well-supported approach for heel pain.
Conclusion
In summary, gastrocnemius recession, while advocated by some, lacks a substantial evidence base to justify its invasiveness. Non-surgical alternatives like PRP have demonstrated promise in treating both Achilles tendinopathy and plantar fasciitis. The decision to undergo this invasive surgery should be made after careful consideration, weighing the available evidence and exploring less invasive treatment options.
Frequently Asked Questions (FAQs)
1. Is gastrocnemius recession the only treatment for heel pain?
No, there are non-surgical alternatives such as platelet-rich plasma (PRP) therapy.
2. How effective is PRP in treating Achilles tendinopathy?
Research suggests that PRP can yield positive outcomes for Achilles tendinopathy, often without the need for surgery.
3. What is the recovery time for gastrocnemius recession surgery?
Recovery can vary, but it is generally longer and more involved than non-surgical options like PRP therapy.
4. Are there any risks associated with gastrocnemius recession?
As with any surgery, there are potential risks, including infection and scarring. Non-surgical approaches carry fewer risks.
5. What should I discuss with my healthcare provider before choosing a treatment for heel pain?
It’s essential to have a comprehensive discussion about your condition, treatment options, potential risks, and expected outcomes with your healthcare provider.
In making decisions about your healthcare, it’s crucial to consider all the available evidence and consult with a qualified medical professional to determine the most suitable treatment for your individual case.